This is an opinion column by Niagara Health Communications Specialist Diane Moore, published in the St. Catharines Standard, Niagara Falls Review and Welland Tribune.
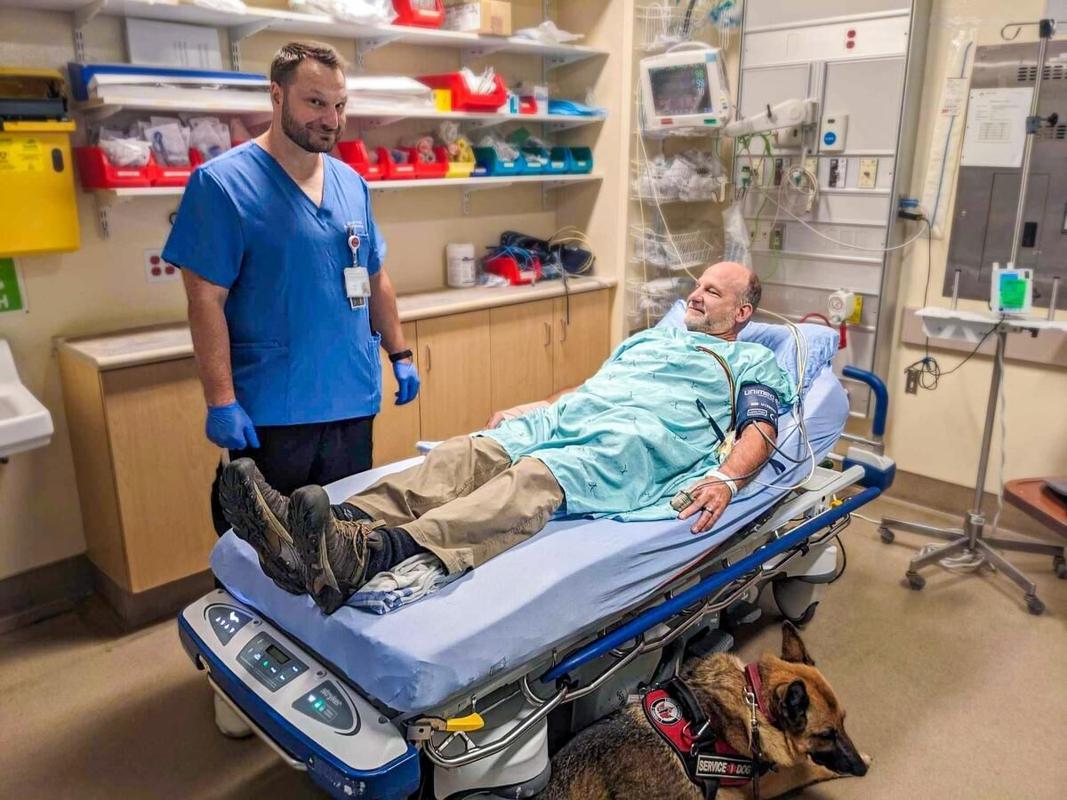
Steve Malone with his son Registered Nurse Jesse Malone and Service Dog Mika at the Niagara Falls ED.
Anxiety and nightmares are some of the symptoms that make life more difficult for people with Post-Traumatic Stress Disorder (PTSD).
For Steve Malone, his service dog Mika is an essential part of his journey to recovery and learning to live with this mental health condition. Mika is by his side when he has to do hard things that trigger his PTSD symptoms, like visiting an Emergency Department (ED).
Malone spent 30 years in paramedicine, saving lives all over the globe through International Medical Missions. The toll of accumulated stress, along with some very traumatic physical and emotional experiences, lead him to a point-of-no-return in paramedicine. Malone says he left his career and has tried to avoid hospitals ever since.
“Being in the emergency department again reawakens some of the physical and emotional trauma I experienced during my career,” he explains. “If I didn’t have PTSD I would go back to doing what I did as a paramedic. I was good at my job and loved what I did. But because of PTSD, I realize I can’t.”
It was a broken wrist on a Friday night in September that brought him back to an ED at the Niagara Falls hospital. Malone had Mika at his side when he needed to have his wrist bone set back in place after falling off of a chair during an odd-job around the house
“Service dogs for PTSD receive intense training for up to 24 months to make us feel secure when we're completely insecure and to provide us comfort and orientation. Mika stayed at my side and did her job. She helped me keep calm as I focused on her and she provided physical contact, which eased my anxiety in a very stressful time.”
But it wasn’t just Mika that made Malone’s visit to the ED a positive one. He says the physicians and nurses at the Niagara Falls hospital provided amazing care.
“I was very impressed with their sense of professionalism,” he says. “From admission to the procedure and casting, everyone was polite, caring, and respectful of me having a service dog. It was not an obstacle for any of them. I was really stunned.”
Meaghan Parker, a Registered Nurse in the Niagara Falls ED, remembers Malone’s visit quite vividly.
“He was afraid that the sedation and procedure would aggravate his PTSD,” she says. “I was very proud of the fact that Steve repeatedly remarked about how the comradery between myself and my coworkers made him feel at ease. That we could provide effective and professional care, while still maintaining a lighthearted and fun environment, is rewarding.”
The ED experience also turned out to be a great learning opportunity for Malone’s son Jesse, a recent nursing graduate and new hire in the Niagara Falls ED.
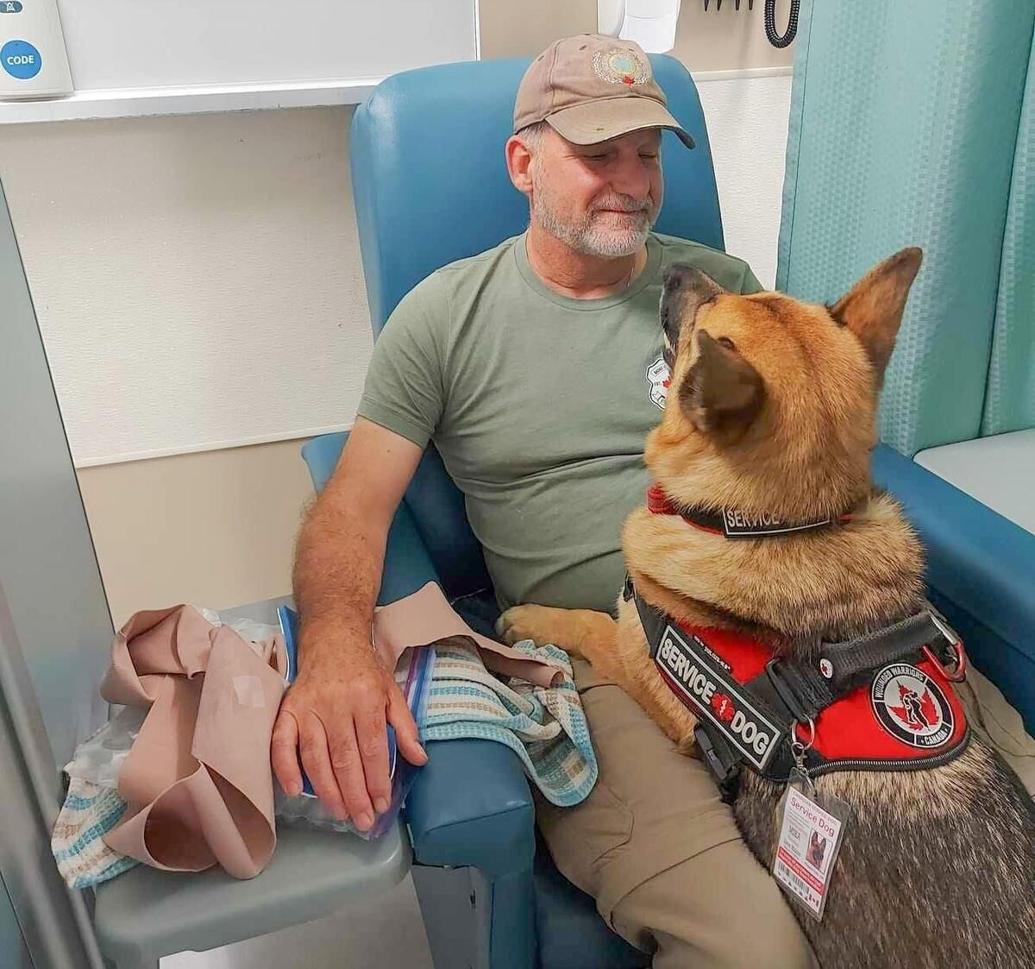
Steve Malone with his Service Dog Mika by his side during a visit to the Niagara Falls ED.
“I was actually pretty busy that night running around with my own patients when my dad came into the ED,” he says. “I pretty much just said, ‘hi dad, what happened?’”
Jesse Malone does not normally work in the area where conscious sedations are performed. That day, he got to sit in and watch. It was a great experience for him to be able to be there for his dad while also learning something new.
Relatively new to healthcare, Jesse Malone was a cook for 12 years before deciding to become a Personal Support Worker. After four years in that role, he went back to school during the pandemic and graduated in March as a Registered Practical Nurse, now working in the ED.
“It is a busy, fast-paced place to work, but everyone is so supportive,” he says. “Service dogs are always welcome here and we will always do our best to accommodate them and offer support to people with PTSD or other mental health conditions.”

For Parker and Jesse Malone, and many other nurses at NH, what keeps them going is having each other to lean on while working in the intensely busy ED.
“We all continue to come to work in this high-stress and sometimes seemingly impossible job because of the amazing people we work with,” says Parker. “Most of us consider our coworkers as not just friends, but our second family. And I think Steve could see this reflected in our interactions during the procedure. We lift each other up and support each other and I'm happy to see that patients can see and feel this when they receive care here.”
“The healthcare system may not be perfect,” Malone admits, “but, I tell you from experience, we are blessed in our country.”
If you have a positive patient story to share about Niagara Health, please contact Diane More at diane.moore@niagarahealth.on.ca.

