I am Niagara Health - Annual Report 2017/18
Share This Page
Share This Page
Research & Academics | How we are doing | Extraordinary Year | Financial Overview | Read online | Get your copy Obtenez un exemplaire | Sign-up for updates | Provide your feedback

We chose the theme I am Niagara Health to highlight how our people are committed to deliver on our promise to provide extraordinary caring to our patients and their loved ones.
This past year has presented many opportunities, and we are grateful to our staff, physicians and volunteers for their unwavering dedication to our deep-rooted purpose of caring.
Our report provides an update on the progress we are making implementing our strategic plan initiatives to improve quality and other important work that supports these initiatives.
You’ll also learn about our increasing focus on research and academics, which is transforming healthcare in Niagara, enhancing the patient experience and attracting and retaining the best and brightest to work at Niagara Health.
We’ve had much to celebrate over the past year and take great pride in the care provided by our teams, delivered with caring and compassion.
Learn more about I am Niagara Health


Providing personalized music playlists on iPods is proving to be beneficial to residents in the Extended Care Unit (ECU) at our Welland Site. Residents with cognitive impairments like dementia can sometimes experience agitation and depression. The ECU staff and Brock University students introduced the Music and Memory Program to enhance the quality of life for residents. The program has helped to improve the mood and behaviour of residents and has been effective in reducing incidence of falls by creating more relaxing environments. “It’s amazing when you see someone who really responds to the music and you see their face brighten and their eyes twinkle or a smile comes across their face,” says Lezlie Leduc, the ECU Program and Services Manager. Music and Memory is part of the Interprofessional Education for Quality Improvement Program (I-EQUIP), which pairs students from Brock and McMaster’s School of Medicine - Niagara Campus, with staff from Niagara Health to work together on health system improvement projects.
Photo: ECU Program and Services Manager Lezlie Leduc with resident Herb Thomas, who is part of the Music and Memory Program.

Patients in Intensive Care Units are our sickest patients and are often unable to express when they feel anxious or are in pain. In addition, our teams may have difficulty accurately determining when patients are experiencing confusion, clinically described as delirium. A leading researcher at Niagara Health, Dr. Jennifer Tsang, and Brock University Associate Professor Dr. Madelyn Law are working with our ICU team to identify better ways to predict and manage a patient’s care when they are experiencing one or more of these symptoms. The pain, agitation and delirium (PAD) research is important to enhance care for our patients by reducing the length of time they require this more intensive level of care while also preventing complications. "When we know that delirium is at the root of confusion and agitation, then we can target specific treatments more readily," Dr. Tsang says. Results from the first phase of the PAD study were presented at the European Society of Intensive Care Medicine conference in Vienna in 2017, and three manuscripts have been submitted for publications. Drs. Tsang and Law are now embarking on the second phase of the study, which broadens the research to involve patients’ family members and additional healthcare disciplines.
Photo: Dr. Jennifer Tsang is studying ways to better manage pain, agitation and delirium in Intensive Care Unit patients.

It’s an alarming statistic: Nearly half of patients admitted to Canadian hospitals are malnourished. To combat malnutrition, Niagara Health joined a University of Waterloo study to look at ways to treat and prevent malnutrition for at-risk patients. Malnourished patients, the majority of whom are seniors, experience longer hospital stays and are at higher risk for readmission within 30 days. Now, when admitted, the patients are asked if they are eating less than usual or have lost weight without trying. If they answer yes to the two screening questions, our dietitians will assess and work with them on a nutrition treatment plan. The second phase of the study launches this fall. There will be an increased focus on connecting patients with family health teams and other care providers in the community for continued nutrition care after they are discharged. Marilee Stickles-White, Niagara Health Manager, Clinical Nutrition Services, says the program is also expanding to more units. "If we identify malnourished patients early on in their hospitalization, we can intervene earlier with great success," she says. "We are making a difference."
Photo: Clinical Dietitian Andrea Digweed meets with patient June Annett at our Greater Niagara General Site to discuss dietary needs.


We are collaborating on a number of initiatives that target areas of medication safety, patient flow and quality of care that directly impact every aspect of a patient’s healthcare journey, as well as the work environment for our teams.

We are proud to work with the very best. To support our teams in providing Extraordinary Caring, we need to provide our people with opportunities to develop and learn. Our teams deserve to work in a respectful culture that fosters critical thinking and innovative ideas.

Investing in the future of healthcare through our people, equipment and technology ensures the work we are doing today to improve the quality and safety of healthcare for our patients and families is sustainable into the future.

Ensuring a smooth transition between hospital and community care for our patients requires innovative approaches to healthcare and effective communication. Partnering in the community to keep people healthier, get better, or cope with disease or end of life requires collaboration outside of the hospital.


As a learning organization, we have strong partnerships with our academic partners, including the Niagara Regional Campus of McMaster University’s Michael G. DeGroote School of Medicine. Medical students work alongside and learn from our healthcare teams. Dr. Han-Oh Chung, Niagara Health’s Academic Lead, says: "It’s a privilege to be involved in supporting, mentoring and the growth of future physicians. By shaping care through teaching and education, it helps us provide better care for the community, and it’s a good thing for patients." Photo: Dr. Han-Oh Chung is Niagara Health’s Academic Lead.

Our Acts of Kindness Workplace Challenge is spreading. The idea for the challenge was generated by our Information and Communications Technology team after the launch of our workplace Be Kind Campaign last summer. The department decided to perform 1,000 acts of kindness to encourage our culture of kindness and connect the team to care. Since then, 15 departments have participated in the challenge, performing thousands of acts of kindness in the hospital and in the community. Photo: From left: Manager Jennifer Ricker-Bonin, Lisette Bisson and Sandy Holmes of the Environmental Services team at our Welland Site participated in the Workplace Acts of Kindness Challenge.

Our Venous Thromboembolism (VTE) program received the Excellence in Patient Safety Award by the Canadian College of Health Leaders last June. VTE, the formation of blood clots in the vein, is one of the most common complications of hospitalization. The program focuses on improving daily risk assessment processes for every admitted patient, and starting preventative treatment, if needed. Photo: Debbie Smith is the VTE Project Lead.

We launched Extraordinary U, the Niagara Health Leadership Institute that offers developmental opportunities for our leaders. The program fosters an environment where leaders can acquire knowledge and skills to empower our people to create A Healthier Niagara. Extraordinary U equips our leaders with the knowledge they need to transform the future of healthcare and provide extraordinary caring. Among topics covered so far in courses offered: critical thinking, human dynamics of change and workplace mental health. Our leaders can also participate in courses offered as part of new partnerships with Hamilton Health Sciences and Niagara Region. Photo: Lisa Harnett-Conners, Food Services Supervisor, Kathy Alexander, Manager Financial Operations and Capital and Jeff Wilson, Director of ICT Operations have all benefitted from Extraordinary U.

Our total operating budget for the year was more than $500 million and we ended the year with a surplus of $12,854,500. The surplus will be reinvested to improve our working capital position.
Read the complete financial statements for 2017/2018
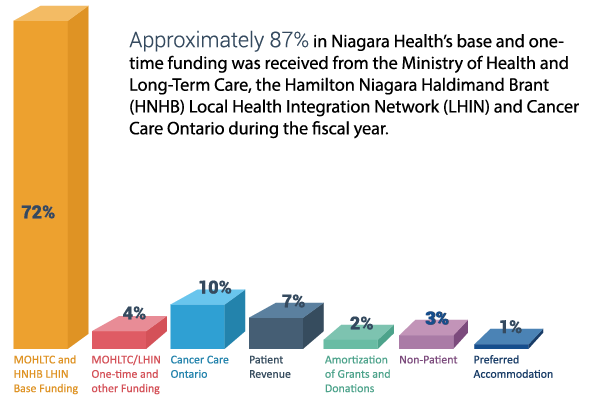
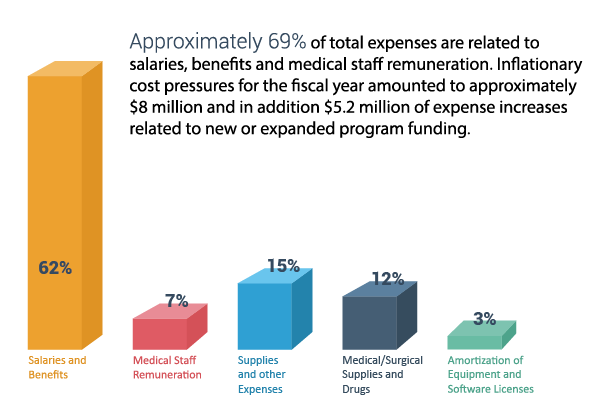
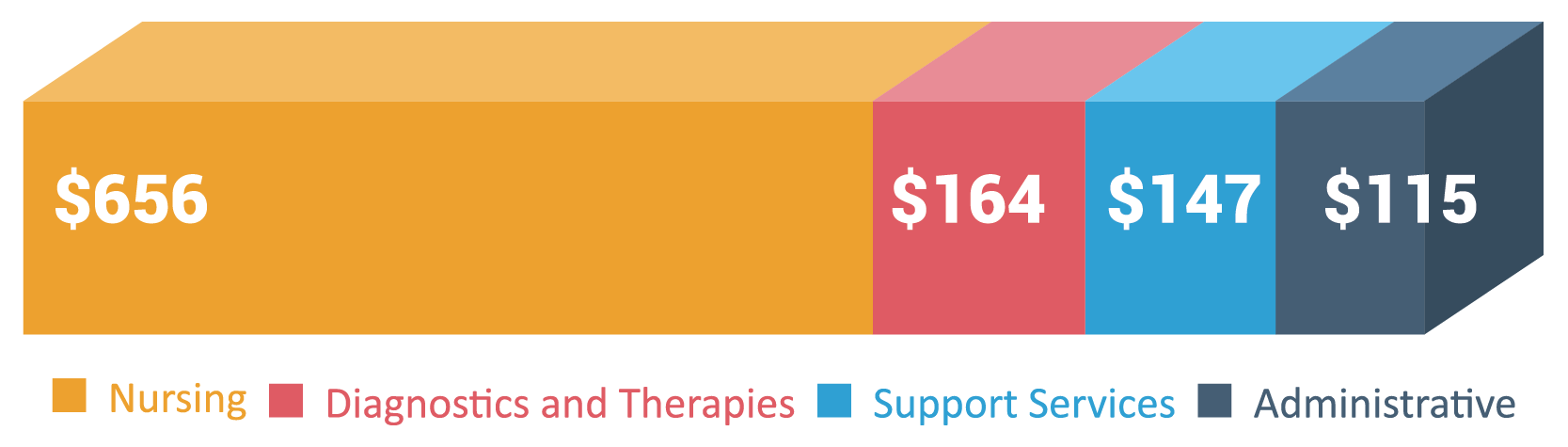
Approximately 79% of expenses are related to direct patient care like nursing, pharmacy, diagnostic imaging, laboratory and therapies. An additional 11% is related to support services like housekeeping, food and maintenance. The remaining 10% is for administrative costs.
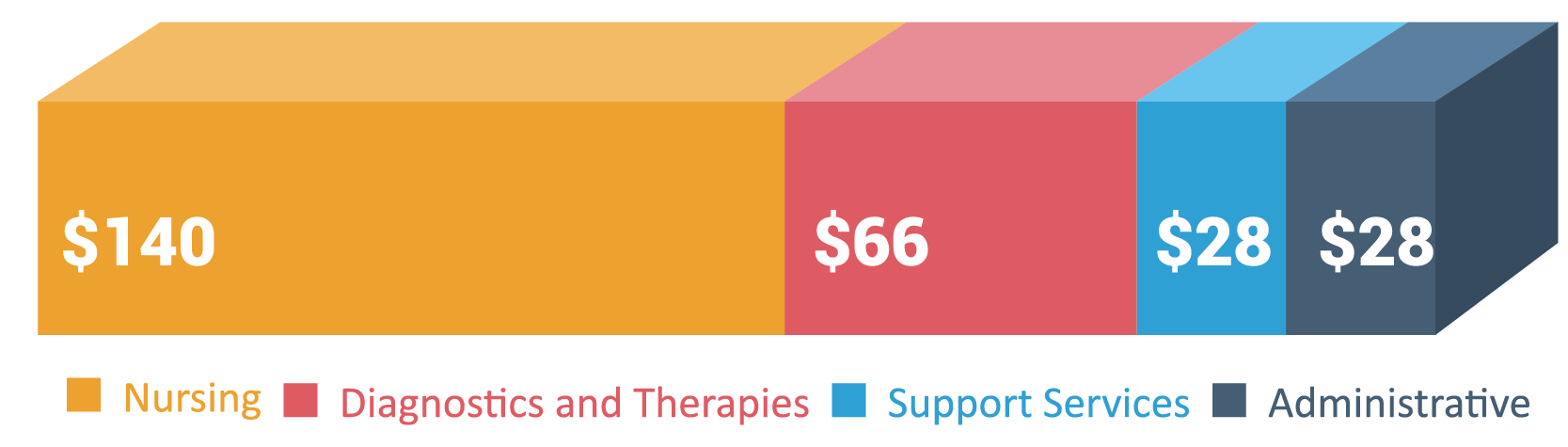
Approximately 79% of expenses are related to direct patient care like nursing, pharmacy, diagnostic imaging, laboratory and therapies. An additional 11% is related to support services like housekeeping, food and maintenance. The remaining 10% is for administrative costs.

949
Beds
34,846
Admissions
7,766
Inpatient
31,467
Outpatient

199,997
Emergency and Urgent Care
68,082
Dialysis/Renal Clinics
38,848
Mental Health Clinics
179,608
Other Outpatient Clinics

2,898
Babies Born
24,410
MRI Scans
5,701
Cataract Surgeries
2,487
Heart Investigation Unit Procedures
* Includes Acute, Complex Care, Long-Term Care, Mental Health and Addictions.
Complete our short survey
